When a mother’s milk disappears for some reason, the only solution to the problem is to feed your baby formula. But there are exceptions to the rule. According to a 2016 study by American scientists, 2-3% of babies turn out to be allergic to formula. More specifically, to the cow’s milk proteins (BMPs) that are part of it.
Infant formula is age-adapted and has a composition that is as close to breast milk as possible. Therefore, most of their ingredients are quickly absorbed and well tolerated by the newborn.
If a baby is allergic to formula, the immune system perceives the proteins in the product as enemy agents and begins to attack them. This releases protective antibodies that are recognized as life-threatening by other cells in the immune system.
Histamine, a mediator of inflammation, comes into the fight to destroy them. That is why the manifestation of an allergy to formula is very similar to a food intolerance, an inflammatory skin disease or even a cold.
This is why very often parents go to extremes and confuse a formula allergy with the usual sweats, respiratory conditions or lactose intolerance. Trusting advice from the Internet, make the wrong assumption that the child has a cumulative allergy to formula.
It can be the other way around: the baby cries after every feeding, but he is still given formula based on cow’s milk proteins.

Symptoms of a formula allergy
There is a list of signs that indicate the presence of an allergic reaction to the formula. These include:
- Excessive gas. It is caused by poorly digested protein, the breakdown products of which cause inflammation of the gastrointestinal tract (GIT).
- Disorders of stools. Stools can be too frequent, with mucus and blood.
- Vomiting after a meal. Babies who are allergic to cow’s milk contained in formula do not eat well and gain weight very slowly.
- Swelling of the lips or mouth.
Therefore, in the presence of a child’s allergy to milk protein, it has:
- diarrhea
- abdominal pain
- vomiting
- respiratory problems (runny nose, cough)
- skin lesions;
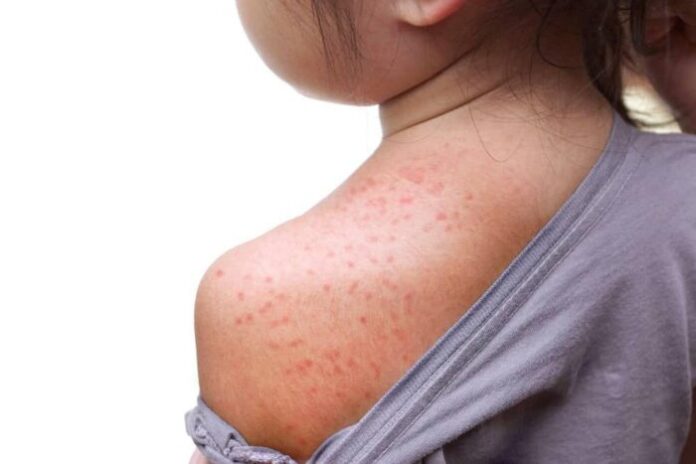
- red rashes that itch and peel.
All of these symptoms usually occur in the first month of life. Apart from these, an infant may suffer from urticaria, laryngeal edema, and sometimes anaphylaxis. The latter, however, is extremely rare in small children.
Cross forms of allergic reactions in children
Much more often, two clinical forms of allergic reaction to baby formula are combined: skin and gastrointestinal.
The first turns out to be a bright red rash with small blisters filled with fluid. Most often the rash appears on the cheeks, forehead, inner parts of the elbows and under the knees. The child tries to cope with the itching and ends up scratching the blisters to a wet crust similar to eczema.
The gastrointestinal form in infants is much more difficult to determine, because the baby cannot talk about it. In addition, such disorders may masquerade as infant colic in the first months of life and be similar to other gastrointestinal diseases.
Allergies to formula may last up to a year, and in some children they may last up to three years. Fortunately, at the age of 3 or 4 years, 99% of children are not allergic to formula at all.
But how do you get through those early years when your baby is diagnosed with an allergy to cow’s milk proteins?

What should you do if your baby is allergic to formula?
If the diagnosis of an allergy to cow’s milk proteins is confirmed, the best treatment is a change in diet.
First, pediatricians advise switching to hydrolyzed formula. On their packaging, it says so: “Blend that should hydrolysates.” In them, the proteins of cow’s milk are fed in a cleaved form and cannot be recognized by the immune system. You can check more about HA formula on organicsbestshop.com.
If there are more severe symptoms, such as severe diarrhea with blood, developmental delays, difficulty swallowing and breathing, the doctor may advise switching to an amino acid-based baby food. Here the protein in general is broken down to a simple, elementary formula, because amino acids are its building material.
Introduce hydrolysates or amino acids in the diet is recommended gradually. They have a specific taste and are not always liked by babies.
If your baby is having trouble gaining weight, pediatricians recommend trying soy-based or goat’s milk formula. They contain very little alpha-s1-casein, which provokes allergies, and with it – bloating, colic and skin rashes. But because of the similarity in the composition of animal milk, most children who are allergic to the proteins of cow’s milk, will not be able to digest both goat’s and mare’s milk as well.
As for soy, it is on the list of the most common food allergens. And sometimes children who are sensitive to BCM can also have hypersensitivity to soy proteins. If your child has no such allergies, adding soy milk to the diet may sensitize the child to it. That is why such mixtures should be introduced in small doses and under the supervision of a doctor.
The best solution therefore remains the use of hydrolyzed mixtures and nutrition based on amino acids.

Allergies to formula or lactose intolerance?
As mentioned above, a true allergy to the formula is very rare. It is often confused with lactose intolerance. In reality, though, these are completely different conditions.
Lactose intolerance is the inability of the gastrointestinal tract of the child to digest the milk sugar lactose. That is, the body lacks the enzyme necessary for this – lactase.
Therefore, intolerance is a digestive enzyme deficiency. In contrast to allergies, in the formation of which the immune system is involved.
Lactase deficiency is more likely if:
- The baby was born underweight (prematurely).
- Both parents suffer from lactose intolerance.
- The baby has had severe diarrhea, causing decreased ability to produce lactase for a week or two.
- The baby has been diagnosed with celiac disease or Crohn’s disease.
If you notice any of the above symptoms in your baby, see your doctor. He will review the family history, since lactose intolerance is most often inherited from parents, and take blood and stool samples.
Remember: children with lactose intolerance do not need hypoallergenic formula. The more so that they cost three times as much and are prescribed for a therapeutic purpose only for a short period of time.

Diagnosis and treatment of allergies to formula
Infants are not suitable for traditional methods of diagnosing allergies, in particular uk tests. Therefore, doctors often use a provocative method: give the baby food containing BCM.
This can be formula and/or a small amount of mother’s milk. The doctor observes whether and what kind of reaction the baby will have.
Another method when a BCM allergy is suspected is to switch the infant to full or partial hydrolysis formula, where the milk proteins are already broken down, or to amino acid-based formula.
When all the symptoms have passed within a week, the child will try to be fed the usual food again. If there are repeated rashes and gastrointestinal disorders, the doctor will be able to confirm that the child is allergic to cow’s milk.
But it is much safer and more reliable to give your child a molecular allergy test. It will show all the allergy variations that exist.
When lactose intolerance is suspected, it can be diagnosed with a special breath test.
Often, lactose intolerance can be seen in parallel with a BCM allergy. That is, these different conditions can be diagnosed in the same child. Therefore, the doctor will have to find a comprehensive solution to treat them.
If a child is found to be lactose intolerant, an enzyme is artificially introduced into her diet. It helps digest milk protein-based formula.









